Turning Science into a Dose: The Story of Formulation
On a cold morning, a small team looks at a tiny vial. Inside is a new molecule that shrank tumors in mice. It works in the lab, but it stings in water, tastes bitter, turns lumpy when mixed, and breaks down in light. A doctor can’t give it as it is, a child won’t swallow it, and a factory can’t make it the same way every time. The science is solid, but it isn’t a medicine yet. Turning that fragile win into something a nurse can measure, a parent can give, and a patient can trust is the job of formulation.

Formulation development turns an active pharmaceutical ingredient into a safe, effective, and manufacturable medicine. It is where pharmacology meets materials science and patient experience: the API must be stabilized, delivered to the right site at the right rate, and presented in a form patients and clinicians can use correctly every time. Whether the goal is an oral tablet, an injectable, or a topical gel, success depends on understanding the API’s behavior in real excipient systems, designing a simple and robust composition–process pair, and proving that performance holds from lab bench to commercial line and through the full shelf-life.
Why it matters: good formulations de-risk late failures, shorten development cycles, simplify tech transfer, and improve adherence. They also widen access—pediatric versions, fixed-dose combinations, modified-release profiles, and device pairing can make the same API usable across populations and care settings.
Connect with our scientific experts for your drug discovery, development and manufacturing needs
What Formulation Development Involves
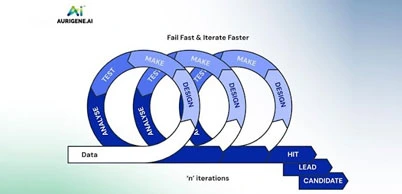
Formulation is a sequence of learn–design–prove loops.
Preformulation and Developability
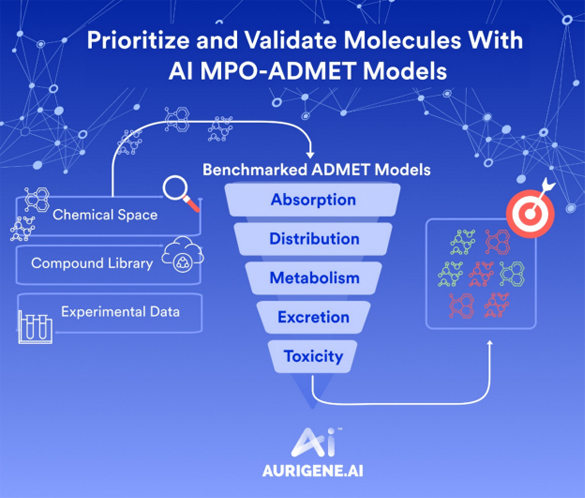
The molecule is examined before any full recipe is chosen. Solubility is mapped across pH, ionization is understood, and solid forms (polymorphs) are checked. Likely breakdown routes—hydrolysis, oxidation, photolysis—are identified so they can be controlled. Permeability and BCS class are profiled to judge oral promise. Excipients are screened for compatibility. For injectables, a sterility approach and endotoxin risk are assessed early. For topicals, partition into skin layers is measured. For inhalation or nasal use, aerodynamic performance and mucosal tolerance are studied. This step shows what the API will tolerate and what it will not.
Target Product Profile and Critical Quality Attributes
The clinical goal is translated into testable features. Assay and impurities define purity; dissolution or release rate sets how fast drug becomes available; particle or droplet size controls performance and stability. Osmolality and pH are set where relevant, and viscosity or rheology is tuned for handling and feel. Dose delivery must be accurate, microbial quality must be safe, container–closure integrity must hold, and in-use stability must be clear. These become the critical quality attributes that guide all later work.

Vehicle and Process Design (QbD)
A practical vehicle and process are designed using Quality by Design. Design of Experiments is used to choose buffers, polymers, surfactants, solvents, and lipids, and to set workable ranges for pH, ionic strength, viscosity, and solid load. A manufacturable process is defined—order of addition, shear, temperature, filtration, and hold times are fixed so results repeat at scale. Modified-release needs matrices or coatings; complex injectables may need emulsions, suspensions, or non-aqueous systems; topicals require a tuned microstructure and acceptable sensory feel. The goal is a simple recipe that behaves well on real equipment.
Analytical and Performance Methods
Tests that truly see change are built first. Stability-indicating assays track the API and its impurities. Physical behavior is characterized through particle or droplet size, zeta potential, and rheology. Performance is measured with dissolution for orals or IVRT/IVPT for topicals. Dose-delivery tests are created for syringes, pumps, droppers, and inhalation or nasal devices so each actuation or mL is reliable. Microbial methods and preservative effectiveness tests are qualified. These methods become the day-to-day language of the product.
Packaging and Device Pairing
The product is matched with the right container and any delivery aid: bottles, blisters, vials, stoppers, tips, pumps, or Blow-Fill-Seal containers; oral syringes, dosing cups, or droppers where needed. Extractables/leachables and sorption are studied so the pack does not steal drug or add anything unwanted. Label claim through shelf-life and in-use is proven. Instructions for use are finalized with human-factors basics such as mL-only dosing and clear color/shape coding of strengths. The pack is part of the product, not an afterthought.
Stability and in-use robustness
Shelf-life is established under ICH conditions across climate zones. Extra stresses—temperature cycling, freeze–thaw, and simulated shipping—are added to expose weak points. In-use periods after opening or reconstitution are defined, and beyond-use dating for clinical settings is set. The aim is a product that survives the real world, not just the storage room.
Scale-up, tech transfer, and validation
The design space is locked and a control strategy is written. Equipment at pilot and commercial scale is qualified so the same microstructure and performance are achieved batch after batch. Process Performance Qualification (PPQ) runs confirm that the process holds. Methods are transferred to QC for routine use. When changes happen, comparability is maintained using the QbD evidence already built.
Regulatory documentation
A clear CMC story is authored that connects the target profile to the chosen control strategy. Excipient choices are justified, release or permeation or dissolution specs are explained, device–product compatibility is shown, and stability claims are supported. The file makes it easy for reviewers to see how risks were identified, controlled, and verified.
Dosage-Form Landscape
Oral dosage forms (solids)
Solid orals cover immediate-release tablets (including ODTs, sublingual and chewable), modified-release systems (matrix, coated, multi-particulate), fixed-dose combinations, hard/soft capsules, mini-tabs and sachets. The development work looks simple on paper but gets technical in the lab. Teams focus on compressibility and flow (so the blend runs clean on the press), control of content uniformity (especially at low dose), and dissolution that is both fast enough and discriminatory. For modified release, polymer choice, pore formers, coating weight gain and matrix geometry matter a lot. Food-effect risk is assessed with biorelevant media and smart dissolution profiles. Patient-centric design shows up in tablet size, scoring, disintegration time, and swallowability. For capsules, shell interactions, fill flow and tamping force are tuned; for softgels, solvent system, shell plasticiser balance, and fill stability are watched closely. Orally disintegrating films and mini-tabs in sprinkles serve paediatric and geriatric needs when swallowing is an issue.

Oral dosage forms (liquids)
Solutions, suspensions, emulsions, reconstitutable powders, syrups and drops are chosen when quick onset, flexible dosing, or paediatric compliance is needed. Core work includes taste-masking (flavours, sweeteners, complexation, or coatings on particles), a good preservative strategy that does not irritate, and tight control of particle or droplet size so dose is uniform from first to last mL. Viscosity is set for pourability and dosing accuracy. In-use stability is proven after multiple openings, shaking, and temperature swings. For unit-dose sticks or ampoules, fill accuracy and seal integrity are critical, with simple instructions that real users can follow.
Parenteral dosage forms
Injectables span aqueous/non-aqueous solutions, suspensions, emulsions, and lyophilised powders for reconstitution. Long-acting depots (oily injections, in-situ forming gels, PLGA microspheres) are a growing class. Development focuses on sterility assurance (aseptic design, sterilising filtration feasibility, or terminal sterilisation where possible), particulate control (visible and sub-visible), osmolality and pH setting, and smart use of antioxidants, chelators and buffers. For lyophilised products, cycle development aims for a neat cake, low residual moisture and clean reconstitution kinetics. Container–closure integrity is proven across storage and shipping. Device metering and usability—vials, prefilled syringes, pens, autoinjectors—are checked early so there is no mismatch at validation.
Ophthalmic, otic, and nasal products
Ophthalmic and otic solutions/suspensions demand low irritation, correct viscosity for residence time, and strict microbial control (sterile or preserved, as appropriate). For nasal sprays (including Blow-Fill-Seal unit dose and multi-dose pumps), plume geometry, spray pattern, droplet size distribution, dose uniformity per actuation and device compatibility are the main levers. Isotonicity, pH drift and preservative effectiveness are tuned so comfort and stability stay balanced.
Inhalation (pulmonary) products
Metered-dose inhalers (MDIs), dry-powder inhalers (DPIs) and nebuliser solutions/suspensions need very tight control of particle size (respirable fraction), aerodynamic performance (impactors), and dose delivery across flow rates. Propellant choice and valve/crimp integrity drive MDI consistency. For DPIs, carrier grade, blending method and humidity control decide if the powder will fluidise and de-agglomerate in the real world. Device–formulation pairing is a project in itself; usability and dose counters reduce use errors.
Topical, dermal, and mucosal products
Creams, ointments, gels, lotions, foams, sprays, pastes, sticks, medicated shampoos—and sterile ophthalmics on the eye—sit under this umbrella. Development centres on Q3 microstructure (emulsion type, gel network, crystal habit), release and permeation behaviour (IVRT/IVPT), and preservative effectiveness without stinging or sensitisation. Dose uniformity per gram or per actuation is proven with simple sampling that regulators trust. Texture, spreadability and feel matter for adherence, and products are checked for climate robustness so they don’t separate or thin out in heat and humidity.
Transdermal patches and topical films
Reservoir and matrix patches, as well as dissolving or mucoadhesive films, deliver steady drug levels without daily peaks and troughs. Work includes polymer selection, adhesive balance (stick without skin damage), enhancer strategy, and flux control through skin models. Cold-flow, edge lift, and wear comfort are evaluated in simple, realistic studies. For films, thickness uniformity, disintegration time and dose per area are verified.
Rectal and vaginal dosage forms
Suppositories, pessaries, foams, gels and vaginal rings are chosen for local therapy or when first-pass metabolism must be avoided. Melting profile or gelation behaviour, leakage risk, patient comfort, and applicator fit are the practical concerns. Microbial limits, osmolality, pH and local tolerance are documented clearly.
Buccal, sublingual, and oromucosal systems
Tablets, films, sprays and lozenges placed in the mouth provide fast onset or avoid the gut. Mucoadhesion, residence time, taste, saliva impact and dose uniformity are optimised together. For sprays, each actuation must deliver the same content even when the patient does not press perfectly.
Implants and long-acting systems
Biodegradable rods, wafers, and in-situ forming depots extend dosing to weeks or months. Polymer grade, molecular weight distribution, residual solvents, and release kinetics (diffusion/erosion balance) are characterised. Surgical handling, swelling, and local tissue response are part of the development story, not afterthoughts.
Device and combination-product fit (cross-cutting)
Across many of these routes, the “device” is half the product. Early human-factors notes, extractables/leachables assessments, dose-metering checks, and climate cycling prevent late surprises. Instructions for use and priming steps are written in simple language and tested with real users, not just engineers.
Formulation Development Services Offered by CDMOs
This section gives a simple, end-to-end view of what a CDMO typically does to turn an API into a stable, patient-ready product.
Early scientific groundwork
CDMOs usually begin with basic scientific checks before touching prototypes. They confirm API identity and purity, look at crystal form and particle size, and see how the material behaves with heat and humidity. Simple tools like DSC and TGA show thermal behaviour. The API is mixed with likely excipients and kept under stress to spot any reaction or colour change. If solubility or stability is weak, salt or co-crystal options are explored. Forced degradation in control strategy is practical and not guesswork.
Formulation design and screening
acid, base, peroxide, heat and light maps how the molecule breaks, so the later Once the fundamentals are clear, the team writes a simple Target Product Profile capturing route, dose, release, shelf-life and pack. A Quality by Design mindset sets the quality attributes, and small design-of-experiments runs help screen excipient levels and process parameters. For poor bioavailability, enabling routes like solid dispersions, lipid systems, nanosuspensions or cyclodextrins are tried. Release is tuned to the clinical need—immediate, extended, delayed or even pulsatile. Taste masking is handled for paediatric and sensitive groups using flavours, sweeteners, resins or light coatings. The same approach works across oral solids and liquids, topicals, sterile injectables, and local routes like ophthalmic, nasal or inhalation, where isotonicity, viscosity and particle size matter a lot.
Device and delivery fit
If the product will finally live in a device, that fit is checked early. For injectables, prefilled syringes or autoinjectors may be preferred. For respiratory, MDI or DPI options are reviewed. Human-factors notes are captured early to avoid rework later. It looks small, but it prevents surprises during validation and routine manufacture.
Prototype development and process selection
At bench scale, multiple prototypes are prepared to meet assay, content uniformity, dissolution or viscosity targets. Process choices are made with care—direct compression versus wet or dry granulation, or enabling routes like hot-melt extrusion, spray drying, bead layering and coating. Dissolution methods are built to be discriminatory and sometimes biorelevant. Where helpful, an IVIVC or lighter IVIVR plan is drafted to connect lab behaviour with expected human performance. Hold-time studies on blends, granules, or bulk solutions make sure the process can actually run in a plant without drama.
Analytical method development and validation
Good formulation fails if analytics are weak. CDMOs build stability-indicating methods for assay and impurities on HPLC or UPLC and validate for accuracy, precision, linearity and robustness. Supporting tests such as residual solvents by GC, water by KF, particle size by laser diffraction, rheology for semisolids, and XRPD/DSC for solid-state are added. Microbiology is covered where relevant—sterility, endotoxin, microbial limits, and preservative efficacy for multidose packs. Methods are then transferred to QC labs with proper protocols and comparison data, not just emails.
Stability and packaging development
Stability and pack are run together. ICH stability studies—accelerated, long-term and sometimes intermediate—are started with clear protocols. Photostability and in-use stability are included where needed. Packaging is chosen after simple risk thinking: blisters (PVC/PVDC, Aclar), alu-alu, HDPE bottles, glass vials or ampoules, prefilled syringes, pumps and droppers. If risk is higher, extractables and leachables are assessed so there are no surprises after launch. Shelf-life and storage conditions are then assigned on honest trending of data.

Scale-up and technology transfer (development to manufacturing)
When the formulation behaves, work moves to pilot and then to the receiving manufacturing site. Mixing energy, granulation endpoints, drying, milling screens, compression speed, coating parameters, and for sterile products, filtration and lyophilisation cycles are defined. Process performance qualification planning starts early, but here the focus is on robust scale-up runs and a clean transfer package: batch records, material specs, critical process parameters, and in-process controls. Cleaning strategies and practical MACO thinking are built into the process from day one.
Sterile and high-potency capabilities within development
Some CDMOs support aseptic development with media fills, sterilising filtration studies, depyrogenation loads, isolators or RABS, and sensible environmental monitoring. For lyophilised products, cycle development targets a sound cake, low residual moisture and reasonable reconstitution time. HPAPI work needs containment, closed transfers, OEL banding and careful cleaning verification. Not every site has these, but where available, sensitive programmes become safer and smoother during development.
Quality systems and development compliance
A working quality system sits behind all of this. Change control, deviations and CAPA, supplier qualification, data integrity, and electronic systems like LIMS or eQMS keep development disciplined. Development reports are written as the work proceeds, not at the end. Reference standards are qualified and tracked, and stability chambers are mapped and monitored. It may feel a bit heavy, but it protects time and reputation later.
Typical development deliverables
Across development you receive a Product Development Report that explains choices, a control strategy with CQAs, CPPs, specs and IPCs, validated analytical methods with transfer reports, stability protocols and summaries with shelf-life logic, a risk register with mitigation steps, and a practical tech-transfer pack ready for the receiving plant. The path is straightforward when run carefully: pre-formulation, rational design, data-driven prototypes, strong analytics, honest stability, right pack, and a tidy handover to manufacturing.
What Aurigene offers
- USFDA-inspected laboratory and manufacturing facilities
- ICH-compliant stability infrastructure with a range of conditions covering multiple climatic zones
- Capability for nasal solutions filled via Blow-Fill-Seal, alongside conventional lines for liquids, lyophilized products, and semi-solids
- End-to-end drug product development for oral, parenteral, and topical dosage forms
- Specialization support for pediatric dosage forms, fixed-dose combinations, and modified-release products
- Development of customized formulations for animals
- Evaluation of container-closure systems, storage, and transportation conditions
- Stability studies aligned to ICH guidance to inform early development decisions
- Development and manufacturing across solid orals (immediate-release, modified-release, fixed-dose combinations, hard/soft capsules, multi-particulates, sachets), oral liquids (solutions with dosing cup, drops with device, suspensions, emulsions), parenterals (liquid and lyophilized injectables, complex injectables, ophthalmic and otic solutions, nasal solutions and sprays), and topical forms (ointment, cream, gel)
- Lifecycle-wide support, from early design through commercialization
- A highly skilled scientific team with deep experience across oral, parenteral, and topical dosage forms
- Experience with advanced formulation technologies applied to complex products
- Tailored solutions designed to optimize development time and cost
- More than 20 years of formulation development experience and a track record of accelerating time-to-market
Common development challenges
Stability versus performance
The solvent, pH, and excipient system that maximizes stability may slow release or worsen taste/feel; trade-offs must be designed, not discovered late.

Scale sensitivity
Shear, temperature history, and hold times change microstructure, particle size, and dissolution; process windows must be real and wide enough.
Device/product interactions
Plastics can sorb actives or preservatives; valves and tips drift; adapters clog; headspace oxygen degrades actives.
In-use behavior
Real caregivers and clinics shake, measure, and store imperfectly; designs must tolerate this.
Globalization
Preservative, sweetener, and colorant rules differ; transport conditions vary; stability claims must fit the hottest route.
Lifecycle agility
Suppliers change and excipient grades drift; a QbD file makes comparability faster and safer.
Future outlook
Model-informed formulation
Solubility–pH and co-solvent models, ripening and droplet-stability models, PBPK/PBBM to tie composition and microstructure to clinically relevant specs.
Preservative-lean designs
Aseptic or ultra-clean approaches, closed systems, unit doses, and hurdle strategies to satisfy safety and consumer expectations.
Smarter devices and human factors
Dose counters, better adapters and tips, and clearer IFUs reduce error; mL-only conventions and strength color-coding become standard.
Advanced packaging and E&L discipline
Low-sorption polymers, improved liners, and earlier, product-specific E&L risk assessments.
Sustainability
Reconstitutable formats, lighter packs, recyclable materials, and transport-savvy stability to cut waste and cost.
Digital quality
Electronic batch records, analytics on PET/dose-delivery/stability trends, and sensorized filling to catch drift early.
Winning formulations keep the science simple and the execution disciplined: choose the fewest excipients that do the job, design a process that locks in performance at scale, pair the product with the right package and device, and prove stability and dose accuracy in the ways patients will actually use the medicine. The craft is consistent across routes—oral, parenteral, or topical—and the goal is the same: a reliable product that patients can trust, from first dose to last.