Clinical Supplies and Pharma Commercial Manufacturing Services
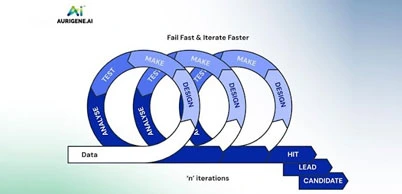
From Discovery to Distribution: How Trusted Manufacturing Sustains Innovation
Clinical supplies and commercial manufacturing sit at the center of a medicine’s practical life. A candidate may be promising in discovery and well profiled in development, but without a dependable path to make, package, label, test, release, and distribute it under good manufacturing practice, the program will stall. This path is not a single handover. It is a continuum that begins with early clinical trial materials and grows into validated, inspected, and globally coordinated commercial supply. Each stage places its own weight on process control, documentation, and regulatory alignment. The science remains important, yet the operational discipline around it becomes equally decisive.

Clinical supplies carry unique demands. They must protect blinding, support randomization, and maintain integrity across varied storage and shipping conditions. Their labels must meet region-specific rules while keeping subjects safe and the data credible. In the European Union this is now framed under the Clinical Trials Regulation, which harmonizes trial processes and defines clear labeling expectations in its annexes. The spirit is consistent across jurisdictions: clinical materials must be traceable, secure, and fit for purpose, with clarity on responsibilities and oversight. These requirements push development teams to translate laboratory methods into robust release and stability programs, and to embed risk-based controls that travel with the product during distribution.
Commercial manufacturing extends these same principles but at scale and under inspection. It relies on clean technology transfer, process qualification, and continued process verification. The technology transfer itself is not a file movement; it is the careful transfer of know-how, ranges, and intent, tested in engineering runs and proven again during validation. Mature CDMOs treat this as a stage-gated exercise with joint ownership between sending and receiving sites. When transfer is handled well, supply chains stay resilient, change control becomes routine, and lifecycle management remains predictable.
Aurigene operates in this space with sites inspected by major regulators and a footprint across Hyderabad and Visakhapatnam. This network supports both clinical and commercial needs, across oral, parenteral, and topical dosage forms. It reflects the industry shift from a cost-first outsourcing mindset to capability-first partnerships that blend development science with manufacturability.
Connect with our scientific experts for your drug discovery, development and manufacturing needs
Overview of Clinical Supplies and Pharma Commercial Manufacturing Services
Clinical supplies represent the transition point where experimental science becomes real-world therapy under controlled conditions. They cover the manufacturing, packaging, labeling, testing, release, storage, and distribution of investigational and auxiliary medicinal products that support clinical studies across phases. Each step is grounded in Good Manufacturing Practice (GMP) and designed to protect the trial’s integrity, patient safety, and data reliability. In early studies, small-batch production may focus on feasibility and quick turnaround, but the same scientific precision applies as the molecule moves forward.

The scope of clinical supply management goes beyond production alone. It includes placebo and comparator handling, design of blinding and randomization strategies, interactive response technology (IRT) integration, returns and reconciliation, and region-specific labeling. Each activity requires careful documentation, not only for compliance but also for traceability, ensuring that every vial, tablet, or blister pack can be traced back through its full history. In the European Union, the Clinical Trials Regulation (CTR) provides a harmonized framework that defines how investigational medicinal products (IMPs) must be prepared, labeled, and monitored under centralized oversight. Despite this harmonization, expectations for safety, data quality, and product integrity remain stringent. In the United States and other regions, FDA, MHRA, TGA, and other agencies enforce equivalent frameworks emphasizing subject protection, robust data collection, and consistent manufacturing control. Together, these frameworks form the backbone of ethical, scientific, and regulatory assurance for clinical materials.
Commercial manufacturing services build upon these same scientific foundations but extend into scale, reproducibility, and market sustainability. Once a molecule demonstrates efficacy and safety, the production process must evolve into a validated, economically viable, and regulatory-inspected system. This transition includes scale-up, process performance qualification (PPQ), method validation, cleaning validation, container closure integrity (CCI) programs, stability management, and regulatory documentation for global submissions. At this point, every control parameter becomes a data-driven decision, with process analytical technologies (PAT) and continued process verification (CPV) forming the backbone of ongoing assurance. Mature CDMOs (Contract Development and Manufacturing Organizations) maintain multi-site networks with harmonized quality systems to ensure redundancy, risk management, and supply continuity. Such systems rely heavily on well-structured knowledge transfer, validated automation, and a lifecycle approach to process control that begins long before market launch.
Good Manufacturing Practice Across the Continuum
The same GMP logic governs both the first engineering batch and the millionth commercial pack. What evolves is not philosophy but granularity and depth. Early in development, process understanding may depend on a few laboratory parameters, such as blend uniformity, dissolution rate, or residual solvent content. As development advances, these parameters are formalized into critical process parameters (CPPs) and critical quality attributes (CQAs) that define the product’s control strategy. Statistical process control, trend analysis, and design of experiments (DoE) help map the design space, a scientifically justified region where the process consistently produces acceptable product quality.
Documentation and traceability deepen with every step. Batch records, analytical raw data, and deviation logs evolve into validated electronic systems that can withstand inspection at any global regulatory level. Risk management frameworks such as ICH Q9 are applied to prioritize controls and allocate testing where it matters most. Rather than testing quality into the product, GMP ensures that quality is built in from the start, an approach known as Quality by Design (QbD). In practice, this means correlating material attributes, process conditions, and performance outcomes through statistically proven relationships. Over time, the result is a manufacturing process that is both reproducible and flexible within defined scientific boundaries.
Clinical Trial Integrity and Labeling
Clinical packaging and labeling are scientific and ethical safeguards. Accurate labeling ensures correct allocation of treatments, preserves randomization, and prevents unintentional unblinding. A small printing error or misplaced label can compromise an entire trial, making label control a high-stakes activity governed by detailed regulations. Under the EU Clinical Trials Regulation, labels must specify product code, dosage, route, storage, batch number, and expiry in a standardized format that maintains blinding but allows for emergency unblinding when necessary.

From a technical perspective, labeling involves validated artwork systems, multilingual layout checks, barcode and serialization control, and tamper-evidence verification. Clinical programs often standardize to the strictest global labeling standard to minimize variation and risk. For global studies, managing label updates across multiple depots and languages requires close coordination between supply, regulatory, and clinical operations, a logistical exercise that rests on sound data and process discipline. In every case, the goal remains the same: preserve the chain of identity and integrity from manufacturing line to patient arm.
Technology Transfer as Knowledge Transfer
Technology transfer is more than moving documents or equipment; it is the scientific translation of process understanding from one site to another without loss of meaning or control. A well-executed transfer includes detailed process maps, material specifications, analytical methods, historical deviations, and justification for each parameter range. The receiving site must absorb not only the “what” and “how” but also the “why,” the rationale behind development decisions.
Scientifically, this ensures that the critical process parameters and control limits derived during development are faithfully preserved during scale-up. Engineering batches serve as controlled experiments that confirm process equivalence and identify scale-dependent effects such as mixing efficiency, heat transfer, or filtration capacity. Advanced modeling tools like computational fluid dynamics (CFD) or residence time distribution (RTD) analysis are increasingly applied to simulate these transitions. When executed properly, technology transfer becomes a process of knowledge continuity, ensuring that the product’s therapeutic and physicochemical identity remain consistent as manufacturing scales and shifts locations.
Container Closure Integrity and Sterility Assurance
In sterile and preservative-free products, the container closure system (CCS) is the primary barrier protecting the product from microbial ingress, moisture, and gas exchange. Scientific validation of this barrier involves container closure integrity (CCI) testing, which provides measurable assurance that the closure performs as designed throughout shelf life. CCI testing may use deterministic methods like helium leak, vacuum decay, or high-voltage leak detection, offering quantitative results far more reliable than older probabilistic dye ingress tests.
Sterility assurance relies on a validated aseptic process supported by environmental monitoring, media fills, and line qualification. For parenteral products, the Sterility Assurance Level (SAL), typically 10⁻⁶, defines the acceptable probability of a non-sterile unit. Integrating CCI data with sterility assurance programs reduces redundant testing while strengthening scientific confidence. Regulatory guidance now allows certain stability time points to rely on CCI data instead of full sterility tests, provided the initial validation demonstrates robust closure performance. This combination of mechanical testing and microbiological control represents the modern scientific standard for sterile manufacturing.
Stability and Lifecycle Control
Stability studies form the scientific basis for determining a product’s shelf life and storage conditions. They measure how chemical, physical, microbiological, and performance parameters change over time under defined conditions of temperature and humidity. For clinical supplies, short-term stability data are often sufficient to support use within a study duration, but commercial products must meet ICH Q1A (R2) and related guidelines for long-term, intermediate, and accelerated stability.
Testing typically includes assay, impurities, dissolution, pH, viscosity, particulate content, and microbial limits, depending on dosage form. Data are statistically analyzed using regression models to estimate expiry dates and establish retest intervals. For biologics or temperature-sensitive products, cold chain stability and in-use stability (after reconstitution or opening) are added to capture real-world conditions. Modern programs integrate predictive stability modeling using Arrhenius kinetics or empirical machine learning to forecast degradation and optimize packaging.
Lifecycle control continues after market approval through ongoing stability studies and annual product reviews, which monitor consistency across lots and materials. When formulations, processes, or packaging change, comparability studies and bridging data ensure that the product remains within its original quality profile. Stability is not a one-time test; it is a continuous dialogue between formulation, process, and environment that sustains confidence in the product’s safety and efficacy throughout its commercial life.
General Offerings of CDMOs in Drug Product Characterization Studies and Testing Services
Method Development and Validation
CDMOs build analytical methods that see the product clearly and withstand routine use. Validation covers specificity, precision, accuracy, linearity, range, robustness, and stability-indicating behavior. For complex products such as suspensions, emulsions, or lyophilized injectables, methods extend to particle size, polymorph form, reconstitution behavior, and viscosity.
Release Testing for Clinical and Commercial Lots
Testing spans identity, assay, impurities, dissolution or disintegration, content uniformity, pH, osmolality, particulate matter, sterility where applicable, endotoxins, and preservative content. Clinical supply release also includes checks related to blinding components and kit completeness. Commercial release layers in process verification data and batch record reviews within qualified electronic systems.
Stability Programs
From short-term clinical programs to ICH long-term, intermediate, and accelerated conditions, CDMOs design phase-appropriate studies. They add in-use stability for multi-dose presentations, photostability where relevant, and transport simulations for cold chain products. Data feed into shelf life, storage statements, and change-control justifications.
Container Closure Integrity and Packaging Qualification
Services include closure choice, torque or crimp optimization, seal integrity testing, extractables and leachables study design, and shipping pack validation. For sterile injectables, CCI becomes a standard part of the control strategy, with methods selected per container and product.
Clinical Packaging and Labeling
Support covers panel creation, booklet labels, multi-language layouts, region-specific content, and comparator management. CDMOs help design blinding strategies and maintain reconciliation through returns. EU programs align to the Clinical Trials Regulation expectations and Annex VI labeling requirements.

Technology Transfer and Process Validation
CDMOs run structured transfers with knowledge capture, engineering batches, and performance qualification. They create validation master plans, execute cleaning validation, and establish continued process verification dashboards once commercialized. For programs moving between fill-finish partners, gap analyses and requalification are standard.
Regulatory and Quality Support
Support includes dossier authoring for sections related to manufacturing and control, responses to queries, and preparation for inspections. For multi-market launches, partners also coordinate regional variations and manage serialization and aggregation where required.
What Aurigene offers
Aurigene provides clinical and commercial manufacturing from sites inspected by major regulators, supported by formulation development and a broad dosage-form footprint across oral, parenteral, and topical categories. The network spans Hyderabad and Visakhapatnam, with capabilities for clinical formulations and commercial supply to global markets.
- USFDA-inspected formulation sites in Hyderabad and Visakhapatnam
- Parenteral manufacturing and development infrastructure in Visakhapatnam
- Equipment set including pilot lyophilizer, bead mill, high-pressure homogenizer, and counter-pressure autoclave
- Global regulatory accreditations across multiple authorities
- Clinical supply manufacturing for oral solids and soft gelatin formulations
- Commercial manufacturing for regulated markets with site approvals
- Packaging and labeling aligned to regional requirements
- Analytical support for release and stability across phases
- Technology transfer and troubleshooting experience over decades
- Capability across oral, parenteral, nasal, ophthalmic, otic, ointment, cream, and gel formats
- Integrated discovery-to-development background within a CRDMO model
- Networked operations across multiple plants for capacity and continuity
Challenges and Future Outlook
Global Compliance and Labeling Complexity
Different regions interpret similar principles with local nuance. The EU’s harmonized clinical framework reduces administrative fragmentation, yet multi-language labeling and evolving guidance still demand careful updates to artwork and pack design. Programs benefit from a single source of truth for label content and controlled templates that adapt to site and country. Continued digitalization of document control will make this cleaner over time.
Technology Transfer at Speed
Pipeline shifts and market dynamics often force transfers midstream. Moving a product between sites or partners without supply risk requires early modular process design, thorough gap analysis, and strong analytical comparability. The sector is converging on standardized data packages and structured knowledge objects to compress transfer timelines while protecting intent.
Sterility Assurance and Closure Integrity
As more injectables and sensitive biologics enter pipelines, sterility assurance becomes even more central. Regulators keep emphasizing science-based integrity testing to complement sterility tests, not replace them. Newer deterministic CCI methods will continue to displace legacy probabilistic tests, improving sensitivity and consistency while supporting faster investigations.

Cold Chain and Distribution Resilience
Clinical and commercial supply chains face variable lanes, ambient challenges, and different last-mile realities. Data loggers and lane qualification are now common. The outlook favors more real-time monitoring, route risk scoring, and passive systems that maintain control without complex infrastructure. For commercial products, serialization and aggregation will keep expanding, creating better visibility but also new data management tasks.
Analytics and Digital Quality Systems
Across the lifecycle, digital batch records, deviation analytics, and trend dashboards help teams see weak signals earlier. Continued process verification becomes more meaningful when fed by structured data from shop floor to stability chambers. The future state points toward integrated platforms that tie lab, manufacturing, and quality data with contextual metadata so that investigations and filings become faster and cleaner.
Capacity and Modality Mix
The industry is balancing mature oral solids with rising demand for sterile injectables and specialty formats. Partners with flexible suites and cross-trained teams will adapt faster. Aurigene’s recent expansion in biologics development and clinical-scale capabilities signals the same direction: broader modality support that can link process and analytics under one roof.
People and Know-how Continuity
Systems and equipment matter, yet capability rests with people who understand failures, edge conditions, and the story behind every range. Retaining and growing this knowledge through structured training, near-miss learning, and communities of practice will remain a defining factor in supply reliability.
Closing Reflection
A strong clinical supplies function protects trial integrity and timelines. A strong commercial manufacturing function protects market continuity and patient trust. When both are built on the same scientific and operational logic, a program moves from early batches to sustained global supply without losing the thread. That is the real marker of quality in this space: not a single perfect run, but a habit of control that survives scale, change, and time.